Newborn Vaccines: What, Why, How, What If
8/1/2026
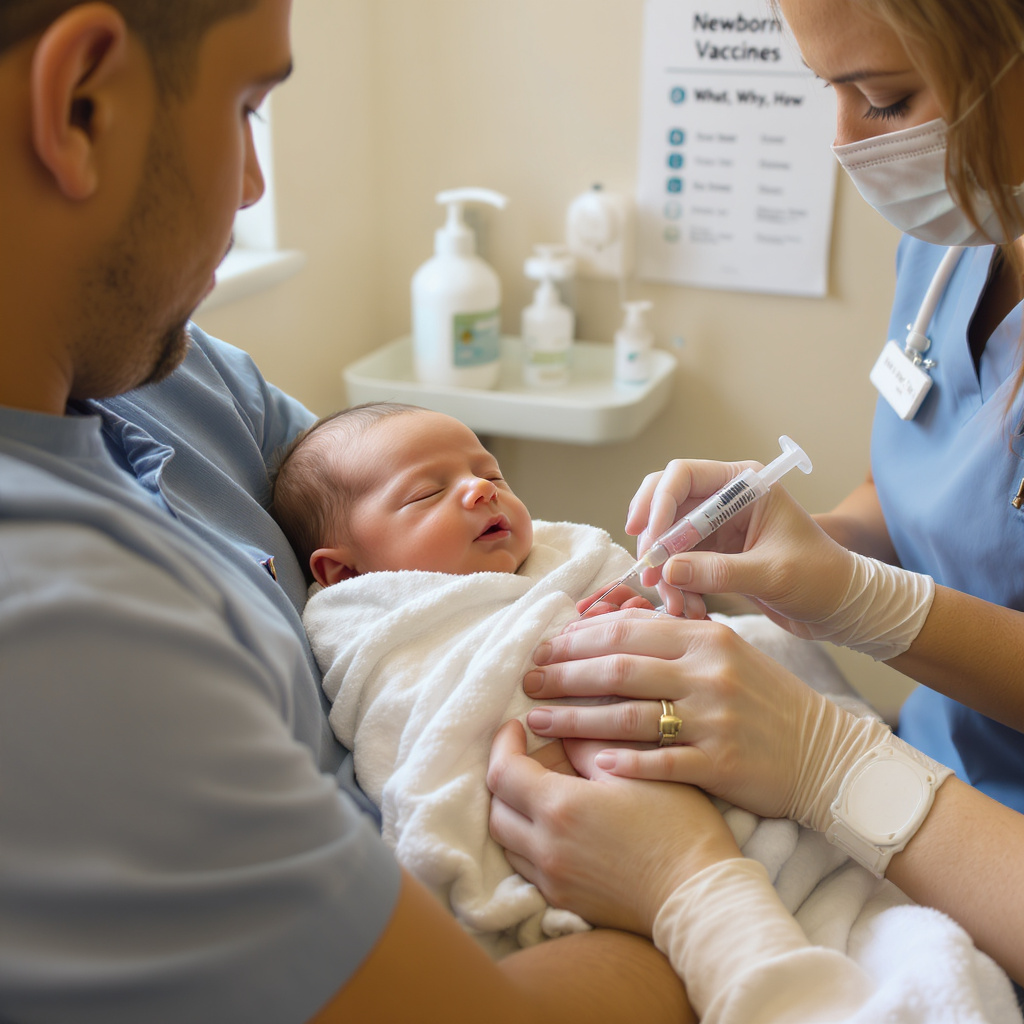
What: Routine newborn and early‑infancy vaccines are doses given to train a baby’s immune system so it can respond to specific germs with less risk of severe illness. Common vaccines in the first year include:
- Hepatitis B — first dose at birth, additional doses around 1–2 months and 6–18 months.
- DTaP (diphtheria, tetanus, pertussis) — series starting at 2 months (typically 2, 4, 6 months).
- Rotavirus — oral series starting at 2 months.
- Hib — begins at 2 months to prevent serious infections.
- PCV (pneumococcal) — usually at 2, 4, 6 months.
- IPV (polio) — starts in early infancy.
- Influenza — yearly from 6 months; first season may need two doses.
- Hep A, MMR, Varicella — commonly begin around 12 months.
Why: Vaccination reduces the chance of severe disease, hospitalization, and complications for babies and helps protect family and community members who may be vulnerable. Most reactions are mild (fussiness, low fever, injection-site tenderness). Serious reactions are rare.
How: Prepare for visits and conversations so you can make informed choices and comfort your baby:
- Bring questions: which vaccines are due, expected side effects, and comfort measures.
- Comfort measures: skin‑to‑skin, breastfeeding, feeding before/after, a cool cloth, and using acetaminophen only if advised by your clinician.
- Record keeping: keep the immunization card, clinic portal record, or state registry up to date and schedule next visits before you leave.
- Combination vaccines & catch‑up: combination shots reduce injections; clinics use catch‑up schedules if a dose is missed.
- Special situations: for NICU or very preterm infants, immune suppression, or prior severe allergic reactions, clinicians will tailor timing and document a written plan in the record and on the baby’s immunization card.
What if: If you delay or choose an alternate schedule, protection is postponed and your baby may be more vulnerable — discuss risks and a personalized plan with your pediatrician. If you want to go further, ask for sources and recent guidance (CDC, AAP, WHO, peer‑reviewed studies). Seek urgent care for difficulty breathing, swelling of the face/throat, seizures, persistent limpness, or very high fever. Keep asking questions; your care team can help translate evidence into a plan that fits your family.
Articles for you

Gentle Baby Massage: Calm Connection (Problem–Agitate–Solution)
Problem: You’re exhausted, your baby is unsettled, and you don’t know a safe, simple way to help—feeds, sleep and colic leave both of you tense and an...

Navigating the Challenges of Infant Colic: Support and Strategies for New Parents
Welcoming a newborn into your life is a joy unlike any other. Amidst the cuddles and coos, however, you may encounter moments that feel overwhelming, ...

Crafting a Birth Plan: Your Personalized Guide to a Confident and Calm Childbirth
Creating a birthing plan is an empowering step for expecting mothers on the path to parenthood. It entails making informed decisions about your childb...